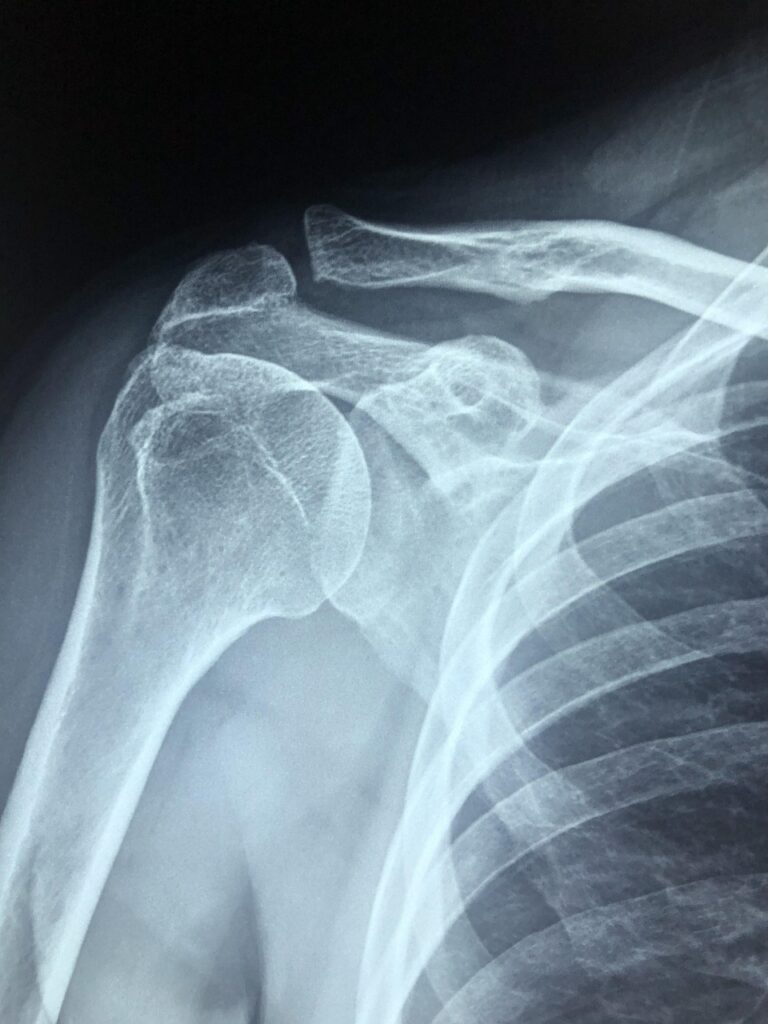
A study from the recent American Arthroscopy Association of North America outlines risk factors for poor outcomes after surgery in patients who have had dislocations.
The Inverted Pear-Shaped Socket and the 25% Critical Size Defect
Background: Steve Burkhart popularized the concept of the inverted pear-shaped socket. He found that if more than 1/4 of the bone was missing from the socket after a dislocation and a strictly soft tissue arthroscopic repair was performed to fix it, then these patients would be at high risk for recurrence of instability. His work established the concept of the 25% critical size defect: if a patient has more than 25% of their socket missing the surgeon should consider augmenting it somehow with bone.
Bone Loss Below the 25% Threshold
This new study takes things a step further. It shows that results after instability surgery tend to be worse in direct proportion to the amount of bone loss one has even below the 25% threshold.
This study is extremely interesting. What we are finding out now with the use of very specific outcome measures is a much more detailed view of how our patients are faring after specific procedures. As we pointed out in our last post just because someone has not requested another operation or had a full redislocation after shoulder instability surgery doesn’t mean that their shoulder is perfect. And this study proves that even subtle bone loss- below the 25% threshold- contributes to that.
Surgical Decision-Making: What Action Do We Take?
As surgeons and patients the question always comes down to what do we do? What action do we take? And as importantly, what action do we NOT take?
Most shoulder surgeons will tend to address bone loss by doing an operation such as a Laterjet procedure or other “bone block” procedure if we judge a defect to be a “critical size” defect. Deciding what is “critical size” is not always clear cut. There are many factors to consider such as whether you are a contact athlete, whether you have failed other procedures, or whether the ball part of the joint (humeral head) locks or engages in the socket.
Bone Block Procedures and Surgeon Approach
Some surgeons will do a bone block procedure for nearly ALL instability cases. This tends to be more common in Europe. The advantage of doing this is that the surgeon gains a tremendous amount of experience in what is a very technical procedure. The disadvantage is that it may be a riskier operation.
Take-Home Point for Patients
The take-home point for patients is that if you have a shoulder dislocation it is very important for your doctor not only to evaluate the amount of bone loss you may have but to be skilled at restoring that bone loss.
